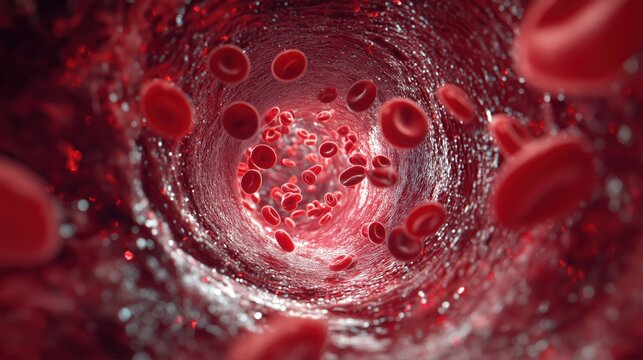
Imagine a vast, intricate network of pipelines stretching over 60,000 miles throughout your body—enough to circle the earth more than twice. This network is your circulatory system, composed of blood vessels. Now, imagine the specialized material lining the inner surface of every inch of these pipes. This lining is not a passive, inert plastic; it is a living, dynamic, and incredibly active layer of cells known as the endothelium. The individual cells that make up this layer are called endothelial cells.
Far from being just a simple cellophane wrapper for your blood vessels, the endothelium is now recognized as a complex and essential “organ” in its own right. It plays a critical role in virtually every aspect of cardiovascular health and disease.
What and Where Are They?
Endothelial cells are a type of epithelial cell (cells that line surfaces) that specifically form the tunica intima, the innermost layer of all blood vessels—arteries, veins, and tiny capillaries. They also line the interior of the heart (the endocardium) and the lymphatic vessels.
Under a microscope, a single endothelial cell is typically thin, flattened, and polygon-shaped. They are connected to one another by specialized structures called cell junctions, which can be tight or loose depending on the function of the blood vessel. But their true power lies not in their individual appearance, but in their collective function as a continuous, selectively permeable barrier.
The Multitude of Functions: More Than Just a Barrier
The endothelium is a master multitasker. Its functions can be broken down into several key areas:
1. The Selective Barrier and Gatekeeper:
This is its most fundamental job. The endothelium physically separates the blood from the surrounding tissues. However, it’s not a solid wall. It’s a dynamic, semi-permeable membrane that meticulously regulates the exchange of substances.
- In capillaries, where this exchange is most critical, endothelial cells allow oxygen, carbon dioxide, water, and small molecules to pass through easily.
- In the brain, the endothelial cells are packed extremely tightly together, forming the blood-brain barrier. This fortress-like lining protects the delicate neural tissue by strictly controlling what enters, allowing only essential nutrients like glucose to pass while blocking toxins and pathogens.
2. The Master Regulator of Blood Flow (Vascular Tone):
Endothelial cells are the body’s traffic controllers for blood. They constantly monitor the blood and the vessel wall, and in response, they release powerful chemicals that signal the surrounding smooth muscle cells to either relax or contract.
- Vasodilation (Widening): The most famous of these chemicals is nitric oxide (NO) . When endothelial cells sense increased blood flow (shear stress) or specific signals like acetylcholine, they produce NO. This gas diffuses to the underlying smooth muscle, telling it to relax. This widens the vessel, lowers blood pressure, and increases blood flow.
- Vasoconstriction (Narrowing): Conversely, they can release chemicals like endothelin-1, which cause the smooth muscle to contract, narrowing the vessel and increasing blood pressure.
3. The Guardian Against Clotting (Hemostasis):
Blood must remain fluid to circulate, but it must also be able to clot to prevent us from bleeding out after an injury. The endothelium is central to balancing these two opposing needs.
- Under normal, healthy conditions, the endothelial surface is anti-thrombotic (anti-clotting) . It is coated with molecules that prevent platelets from sticking to the vessel wall and inactivates the coagulation cascade. This ensures blood flows freely.
- When a vessel is injured, the endothelial cells at the site switch to a pro-thrombotic (pro-clotting) state. They release molecules that activate platelets and clotting factors, quickly forming a clot to seal the wound and stop the bleeding. Once the injury is repaired, they switch back to their anti-clotting state.
4. The Conductor of Inflammation and Immune Response:
When a pathogen invades a tissue or an injury occurs, the body needs to send immune cells to that specific spot. Endothelial cells act as the signposts and gateways for this process.
- Upon detecting inflammatory signals (like histamine or cytokines) from the injured tissue, endothelial cells in the nearby blood vessels express sticky proteins called adhesion molecules on their surface.
- White blood cells (leukocytes) rolling along in the bloodstream see these signals and begin to stick (adhesion). The endothelial cells then gently pull apart their junctions, allowing the white blood cell to squeeze through the vessel wall and into the tissue to fight the infection—a process called extravasation.
5. The Architect of New Vessels (Angiogenesis):
When tissues grow, need more oxygen, or are healing, they require new blood vessels. Endothelial cells are the architects and construction workers of this process, called angiogenesis.
- In response to signals like vascular endothelial growth factor (VEGF), endothelial cells exit their quiet, resting state. They begin to proliferate (multiply), migrate toward the signal, and organize themselves into hollow tubes. These tubes then connect with other tubes to form a new, functional capillary network. This is crucial for development, wound healing, and the female reproductive cycle.
When the Endothelium Fails: The Root of Disease
Given its central role, it’s no surprise that a dysfunctional endothelium is a hallmark, and often the starting point, of many major diseases. This state is called endothelial dysfunction.
The primary cause of endothelial dysfunction is chronic, low-grade inflammation and oxidative stress, often driven by modern lifestyle factors like smoking, a poor diet, lack of exercise, and stress. High blood pressure, high cholesterol (especially oxidized LDL), and high blood sugar (diabetes) are also major attackers.
When the endothelium is damaged and dysfunctional, its carefully balanced systems tip toward chaos:
- It produces less nitric oxide, leading to chronic vasoconstriction and high blood pressure.
- Its surface becomes sticky and pro-thrombotic, increasing the risk of dangerous blood clots.
- It becomes more permeable, allowing harmful LDL cholesterol to penetrate the vessel wall.
- It expresses more adhesion molecules, drawing in inflammatory immune cells.
This cascade of events is the foundation of atherosclerosis, the hardening and narrowing of arteries. The buildup of cholesterol, immune cells, and cellular debris (plaque) within the artery wall is the body’s flawed attempt to heal the initial endothelial injury. A ruptured plaque can then trigger a massive clot, leading to a heart attack or stroke.
In summary, endothelial cells are far more than a simple lining. They are a dynamic, sensory, and regulatory organ that tirelessly works to maintain the health of our blood vessels and every organ they supply. Protecting our endothelium through a healthy lifestyle is one of the most effective ways to protect our overall health and prevent cardiovascular disease.