Utopedia Legendary Entry | A Deep-Knowledge Article
Prologue: The Memory That Vanished
In November 1901, a 51-year-old woman named Auguste Deter was admitted to the Municipal Mental Asylum in Frankfurt, Germany. Her husband brought her there because something had gone terribly wrong with the woman he married. Auguste had become suspicious of everyone around her, accusing her husband of infidelity without cause. She hid objects and forgot where she placed them. She became disoriented in her own home. When she spoke, she would start a sentence and then trail off, unable to find the words to finish[1].
A young doctor named Alois Alzheimer took a particular interest in Auguste’s case. He interviewed her extensively, and his notes preserve one of the most poignant exchanges in medical history:
“What is your name?” he asked.
“Auguste.”
“Your last name?”
“Auguste.”
“What is your husband’s name?” he pressed gently.
“Auguste, I think.”
When he asked her to write her name, she tried but stopped midway, saying, “I have lost myself.”
That phrase—“I have lost myself”—captures the essence of what we now call Alzheimer’s disease better than any textbook definition ever could. Auguste Deter was not just losing her memory; she was losing the very threads that wove together the tapestry of her identity. And in her brain, invisible to anyone at the time, two tiny protein fragments were slowly accumulating, destined to form the plaques and tangles that would bear Dr. Alzheimer’s name for eternity[2] .
This is the story of those protein fragments, of the brain they inhabit, and of the millions of lives they touch. It is a story of scientific discovery, of molecular mischief, of genetic destiny and lifestyle choice—and of the relentless human quest to understand why some minds fade while others burn bright until the very end.
Part I: The Architecture of Memory
The Three-Pound Universe
To understand Alzheimer’s disease, we must first understand its canvas: the human brain.
Hold your hands cupped together. That is roughly the size and weight of the organ that contains everything you are—every memory of your childhood home, every skill you’ve ever learned, every person you’ve ever loved, every word of every language you speak, every song you know by heart, every hope, every fear, every dream. Three pounds of tissue. Eighty-six billion neurons. And a connection density that makes the internet look like a child’s string game.
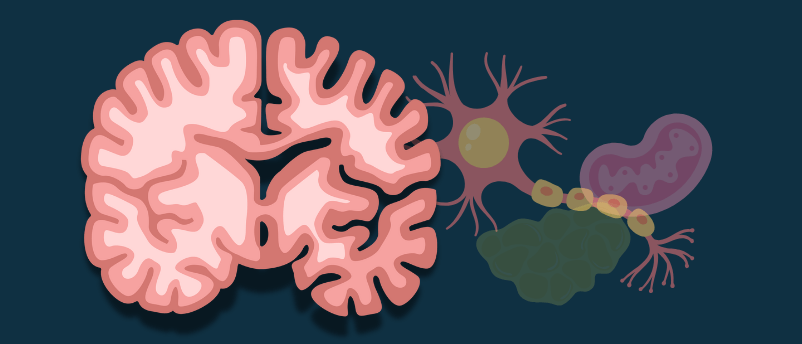
The brain is not a uniform blob. It is a precisely organized architecture with specialized regions handling specialized tasks. At the heart of memory and learning sits the hippocampus, a seahorse-shaped structure buried deep in the temporal lobe. The hippocampus is the brain’s librarian—it decides which experiences are worth encoding into long-term memory and helps file them away for future retrieval[3].
Surrounding the hippocampus is the cerebral cortex, the wrinkled outer layer that gives the brain its characteristic walnut appearance. The cortex is where higher thinking happens—perception, reasoning, language, complex problem-solving. Different regions of the cortex handle different functions: the frontal lobe manages planning and personality, the parietal lobe processes sensory information, the temporal lobe (where the hippocampus resides) handles auditory information and object recognition[4] .
And connecting it all are the neurons themselves—specialized cells designed to receive, process, and transmit information. A typical neuron looks like a tiny tree: a cell body (the trunk) with branching dendrites (the roots and branches) that receive signals from other neurons, and a long axon (like a cable) that transmits signals to the next neuron in line. The point where one neuron meets another is called a synapse, and it is across these microscopic gaps that the business of thought and memory occurs[5].
The Molecular Scaffolding
Inside every neuron, a complex infrastructure keeps everything running. Two proteins are particularly important to our story, because they become the central villains in Alzheimer’s disease.
Amyloid precursor protein (APP) is a large protein that sits embedded in the neuron’s membrane, with part of it sticking outside the cell and part inside[6]. Think of it as a antenna, receiving signals from the cellular environment and helping the neuron respond appropriately. APP is produced constantly by neurons, vascular cells, and even platelets, and under normal circumstances, it is harmlessly broken down and recycled[7] .
Tau protein is an internal scaffolding specialist[8]. It binds to microtubules—the long, hollow rods that act as the neuron’s internal highways for transporting nutrients, organelles, and signals from the cell body down the axon to the synapse. Tau helps keep these microtubules straight and stable, like railroad ties holding train tracks in place[9].
For decades, these proteins went about their business unnoticed, doing their jobs in the brains of billions of humans across millennia. But in some brains—for reasons we are still working to fully understand—they begin to misbehave. And when they do, the consequences are catastrophic.
Part II: The Discovery—A Peculiar Disease
Dr. Alzheimer’s Patient
When Alois Alzheimer first encountered Auguste Deter in 1901, the concept of “dementia” existed, but it was considered a natural consequence of aging—what we might today call “getting senile.” The idea that memory loss and cognitive decline might represent a specific disease with identifiable physical causes was almost unheard of[10] .
Alzheimer was different. Trained by some of the most innovative neuropathologists of his era—Franz Nissl, who developed staining techniques to visualize neurons, and Emil Kraepelin, who would later name the disease after his colleague—Alzheimer approached mental illness with a pathologist’s eye. He believed that changes in behavior and cognition must correspond to changes in brain structure[11] .
Auguste Deter became his proof.
Over the years following her admission, Alzheimer kept in touch with her caregivers, tracking her decline. By the time of her death in 1906, Auguste had become completely apathetic, unresponsive, lost to the world. Alzheimer arranged for her brain to be sent to him for examination[12].
Using the staining techniques he had learned from Nissl, Alzheimer examined thin slices of Auguste’s brain under his microscope. What he saw was unlike anything described before.
The brain showed dramatic shrinkage—cortical atrophy, the doctors call it. But more striking were the abnormalities at the cellular level. Scattered throughout the tissue were dense, spherical deposits that stained darkly, sitting outside the neurons. And inside many neurons, tangled bundles of thread-like structures occupied spaces where healthy cellular machinery should have been [13].
Alzheimer called the external deposits senile plaques and the internal tangles neurofibrillary tangles. He presented his findings at a psychiatry conference in 1906, but the response was muted. His lecture received only a two-line abstract in the conference proceedings. The scientific community was not ready for the idea that dementia was a disease[14] .
It took four more years, and the influence of his mentor Emil Kraepelin, for the condition to receive a name. In the 1910 edition of his textbook Psychiatrie, Kraepelin coined the term “Alzheimer’s disease” to distinguish this presenile form of dementia from the senile dementia of old age. Even then, the discovery remained obscure for decades[15] .
The Resurrection
Alzheimer’s disease might have remained a footnote in medical history if not for two developments in the latter half of the twentieth century.
First, people started living longer. As infectious diseases and acute illnesses came under control, chronic conditions of aging—including dementia—became more visible and more pressing. Second, new technologies allowed scientists to look more closely at the plaques and tangles that Alzheimer had described[16] .
In 1984, researchers George Glenner and Cai’ne Wong at the University of California, San Diego, isolated the protein that made up the senile plaques. They called it beta-amyloid (Aβ), and they sequenced its amino acid structure, revealing it to be a fragment of the much larger amyloid precursor protein. Two years later, other researchers identified tau as the primary component of the neurofibrillary tangles[17] .
The molecular era of Alzheimer’s research had begun.
Part III: The Villains—Amyloid and Tau
Beta-Amyloid: The Sticky Fragment
Imagine you have a roll of duct tape. Under normal circumstances, you tear off a piece, use it for whatever task you need, and throw away the scrap. But now imagine that instead of being thrown away, those scraps start sticking together—first in small clumps, then in larger and larger accumulations, until eventually you have sticky masses interfering with everything around them.
That, in essence, is what happens with beta-amyloid in the Alzheimer’s brain.
Beta-amyloid is created when enzymes called secretases cut the amyloid precursor protein at specific points. Think of APP as a long string of beads. One enzyme, beta-secretase, makes the first cut at one end. Another enzyme, gamma-secretase, makes a second cut somewhere further down the string. The fragment that gets cut out—the piece between the two cuts—is beta-amyloid[18] .
Depending on exactly where gamma-secretase makes its cut, beta-amyloid fragments come in different lengths. The most common versions are 40 amino acids long (Aβ40) and 42 amino acids long (Aβ42). That difference of just two amino acids matters enormously. Aβ42 is much stickier, much more prone to clumping together (aggregating) than its shorter cousin[19] .
In a healthy brain, these fragments are cleared away by various cellular garbage-disposal systems. But in the Alzheimer’s brain, production outpaces clearance, or clearance mechanisms fail, or both. The fragments begin to accumulate. At first, they form small, soluble clumps called oligomers. These oligomers are particularly toxic—they drift through the brain, interfering with synaptic function, disrupting communication between neurons, and triggering inflammatory responses. Later, the oligomers coalesce into the larger, insoluble plaques that Alzheimer saw under his microscope[20] .
Recent research has revealed something surprising: beta-amyloid doesn’t just accumulate outside neurons. It also builds up inside vulnerable neurons, starting very early in the disease process. A 2025 study found that neurons containing internal amyloid deposits were precisely the ones most likely to die, while neurons that accumulated tau alone survived just fine, even in advanced disease[21] . This suggests that amyloid may be the initial trigger—the spark that lights the fire.
Tau: The Tangled Scaffold
While amyloid is accumulating outside neurons, tau is misbehaving inside them.
Recall that tau’s normal job is to stabilize microtubules—the neuron’s internal transportation network[22]. It does this by binding to the microtubules and keeping them straight. But tau is regulated by phosphorylation, the addition of phosphate groups that act like molecular switches. In its normal state, tau has just enough phosphate groups to do its job without becoming too sticky[23] .
In Alzheimer’s disease, something goes wrong with this regulation. Enzymes add too many phosphate groups—a state called hyperphosphorylation[24]. Hyperphosphorylated tau loses its ability to bind to microtubules. The microtubules fall apart, disrupting transport within the neuron. Meanwhile, the freed tau begins sticking to itself, forming abnormal filaments that pair up and twist around each other[25] .
These twisted pairs are the neurofibrillary tangles that Alzheimer saw. As they accumulate, they fill the neuron’s interior, crowding out essential structures and interfering with function. Eventually, the neuron dies, leaving behind a “tombstone” of tangled protein—a ghost of the cell that once was[26] .
The Deadly Dance
For years, researchers debated which protein was the real culprit—amyloid or tau[27]. The amyloid cascade hypothesis, first proposed in the early 1990s, suggested that amyloid accumulation was the primary event, triggering everything else including tau pathology. The tau camp argued that tangles correlated better with cognitive decline than plaques did[28].
Today, most researchers recognize that both are important and that they interact in complex ways. Think of Alzheimer’s as a two-stage process:
In Stage 1, amyloid begins accumulating silently, perhaps for decades, without causing noticeable symptoms. This amyloid creates a toxic environment—disrupting synapses, triggering inflammation, stressing neurons. It’s like a neighborhood where crime is starting to increase but hasn’t yet become obvious[29] .
In Stage 2, tau pathology spreads through this vulnerable environment. The spread follows a predictable pattern, moving from the transentorhinal cortex (near the hippocampus) to the hippocampus itself, and then outward to the association cortices. As tau spreads, symptoms appear and worsen. The location of the tangles determines the symptoms—tangles in memory areas cause memory loss, tangles in language areas cause word-finding difficulty, and so on[30] [31]
The amyloid creates the kindling; tau lights the fire. And once the fire is burning, the two proteins work together to accelerate destruction.
Part IV: The Brain Under Siege
Beyond the Proteins
While amyloid and tau are the most visible villains, they do not work alone. The Alzheimer’s brain is a battlefield, with multiple forces contributing to the devastation.
Neuroinflammation is a major player. The brain has its own immune cells, called microglia, which act as first responders to injury or infection. In the Alzheimer’s brain, microglia detect accumulating amyloid and tau and activate to clear them. But chronic activation backfires—the microglia release inflammatory chemicals that damage healthy neurons alongside the pathological proteins. Genetic studies have identified variants in microglial genes (like TREM2) that increase Alzheimer’s risk, highlighting the importance of this inflammatory response[32] .
Mitochondrial dysfunction also plays a key role. Mitochondria are the cell’s power plants, generating the energy neurons need to function. In Alzheimer’s disease, mitochondria become damaged and produce less energy while generating more toxic byproducts called reactive oxygen species. This oxidative stress damages cellular components and accelerates degeneration[33] [34]
The blood-brain barrier, normally a tight seal that protects the brain from harmful substances in the bloodstream, becomes leaky in Alzheimer’s disease. This allows toxins and immune cells to enter the brain, further fueling inflammation and damage .
And throughout the brain, synapses—the connections between neurons—are lost. Synapse loss correlates more strongly with cognitive decline than neuron loss itself. Before neurons die, they stop communicating effectively. It’s like a city where the phone lines are down long before the buildings collapse[35] .
Why Some Neurons Are More Vulnerable
One of the most puzzling aspects of Alzheimer’s disease is its selectivity. Not all neurons are equally vulnerable. Some populations—particularly in the hippocampus and certain cortical layers—degenerate early and severely, while others remain relatively intact even in advanced disease.
Recent research has begun to explain why. Vulnerable neurons share certain characteristics. They tend to be long-projection neurons—cells with very long axons that connect distant brain regions. Maintaining these long connections requires enormous energy and complex transport systems, making these cells particularly susceptible to disruptions in mitochondrial function and microtubule stability[36] .
Vulnerable neurons also appear to have higher baseline levels of amyloid production or lower capacity for clearing cellular debris. And they express particular patterns of genes involved in inflammation and protein modification that may predispose them to degeneration when stressed[37] .
Understanding this selectivity is more than an academic exercise. If we can identify what makes neurons vulnerable—or conversely, what protects resistant neurons—we might develop strategies to shield the vulnerable populations from damage.
Part V: The Genetic Blueprint
The Families: Early-Onset Alzheimer’s
For most people, Alzheimer’s disease strikes late in life—after age 65, and increasingly after 85. But a small minority—perhaps 1-5% of cases—develop symptoms much earlier, sometimes in their 30s, 40s, or 50s. These early-onset familial Alzheimer’s cases have provided crucial insights into the disease mechanisms[38] [39].
In these families, the disease follows a clear inheritance pattern: if you inherit the mutation, you will almost certainly develop Alzheimer’s, usually around the same age as your affected parent. Researchers have identified three genes responsible for most cases of early-onset familial Alzheimer’s[40] [41]:
APP (on chromosome 21) encodes the amyloid precursor protein itself. Mutations in APP can increase production of total amyloid, or shift the balance toward the stickier Aβ42 form. The connection to Down syndrome is telling—people with Down syndrome have three copies of chromosome 21 (where APP resides), produce excess amyloid from birth, and almost invariably develop Alzheimer’s pathology by middle age[42] .
PSEN1 and PSEN2 encode presenilin 1 and presenilin 2, components of the gamma-secretase complex that cuts APP to generate amyloid. Mutations in these genes alter gamma-secretase activity, typically increasing the proportion of Aβ42 produced.
These discoveries, made in the 1990s, provided powerful support for the amyloid hypothesis. If mutations in genes directly involved in amyloid production cause early-onset Alzheimer’s, then amyloid must be central to the disease process[43] .
The Risk Factor: APOE
Most Alzheimer’s cases, however, are not caused by deterministic mutations. Instead, they reflect a complex interplay of genetic risk factors and environmental influences. The most important genetic risk factor by far is apolipoprotein E (APOE)[44] [45] [46].
APOE comes in three common variants, or alleles: ε2, ε3, and ε4. Everyone inherits one allele from each parent, so possible combinations include ε2/ε2, ε2/ε3, ε3/ε3, ε3/ε4, and ε4/ε4. The ε3 allele is most common, carried by about 60% of the population. The ε4 allele is carried by about 15-25% and has very different effects depending on whether you have one copy or two[47] [48].
Compared to people with the common ε3/ε3 combination:
- People with one ε4 copy have about 3-4 times the risk of developing Alzheimer’s
- People with two ε4 copies (ε4/ε4) have about 8-12 times the risk
The ε2 allele, by contrast, appears protective, reducing risk compared to ε3[49] [50].
APOE’s role in the brain is complex. The protein helps transport cholesterol and other lipids, but it also influences amyloid clearance. The ε4 variant is less effective at clearing amyloid than ε3 or ε2, leading to greater accumulation. It also affects inflammation, synaptic function, and many other processes relevant to Alzheimer’s[51].
Importantly, APOE ε4 is a risk factor, not a guarantee. Many ε4 carriers never develop Alzheimer’s, and many people without ε4 do. Genetics loads the gun, but environment and lifestyle pull the trigger—or don’t.
The Other Risk Genes
Beyond APOE, genome-wide association studies have identified dozens of other genetic variants that influence Alzheimer’s risk, each with a small effect. Many of these variants cluster in pathways already implicated in the disease[52] :
- TREM2, CD33, and other microglial genes highlight the importance of inflammation
- ABCA7 and SORL1 are involved in lipid metabolism and amyloid processing
- CLU (clusterin) and PICALM affect amyloid clearance and synaptic function
The picture emerging is of a disease with multiple routes of entry. Some people may have a genetic predisposition toward excess amyloid production. Others may have less efficient clearance systems. Others may have overactive inflammatory responses. All these pathways can converge on the final common path of neurodegeneration[53] [54].
Part VI: The Long Goodbye—Stages and Symptoms
The Silent Phase
Alzheimer’s disease begins decades before the first symptom appears. This preclinical phase is a time of silent accumulation—amyloid slowly building up in the brain, microglia gradually becoming chronically activated, synapses quietly being lost. The brain compensates, drawing on its reserves of cognitive reserve—the buffer created by education, mental stimulation, and lifelong learning. Symptoms remain absent because the brain has enough redundancy to work around the damage[55][56]data-cite-text=”https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024″ [56]class=”js–wpm-format-cite”> [56]
How long does this silent phase last? Estimates vary, but amyloid accumulation may begin 15-20 years before symptom onset. This long preclinical window offers a crucial opportunity for early intervention—if we can identify who is accumulating pathology and stop it before symptoms appear[57] .
Mild Cognitive Impairment
The first noticeable changes fall under the category of mild cognitive impairment (MCI) , particularly the amnestic form that affects memory. At this stage, problems are noticeable to the individual and close family members but don’t significantly interfere with daily life[58] .
The person might:
- Forget recent conversations or events more frequently
- Have trouble remembering appointments or planned activities
- Misplace items and struggle to retrace steps
- Have increasing difficulty finding words
- Feel overwhelmed by complex tasks like managing finances or following detailed instructions
Not everyone with MCI progresses to Alzheimer’s. Some remain stable, and some even improve if their cognitive issues have other causes (medication side effects, depression, vitamin deficiencies). But in a significant proportion, MCI is the earliest clinical manifestation of Alzheimer’s disease[59] .
Mild Alzheimer’s Dementia
As the disease progresses, cognitive problems become more pronounced and begin to interfere with independent function. This is the threshold where MCI crosses into dementia.
Memory loss becomes more severe, particularly for recent events. The person may repeat questions or stories within the same conversation. They may get lost in familiar places or have trouble following directions. Personality changes may emerge—the easygoing person becomes irritable, the cautious person becomes suspicious[60] .
Language problems intensify. Finding the right word becomes a constant struggle. Conversations may become simpler, with more circumlocution (talking around a word the person can’t retrieve). Reading comprehension declines.
Executive functions—planning, organizing, problem-solving—become impaired. The person may have trouble following a recipe, managing medications, or keeping track of bills. Judgment may be compromised, leading to uncharacteristic decisions[61] .
Moderate Alzheimer’s Dementia
In the moderate stage, the disease spreads more widely through the brain, affecting more cognitive domains and beginning to impact basic functions.
Memory loss now extends to personal history. The person may not recall their address, phone number, or the names of family members. They may not recognize familiar faces at times. Disorientation to time and place is nearly constant—they don’t know the day, date, or where they are.
Behavioral and psychological symptoms often emerge or intensify. These can include:
- Agitation and aggression, sometimes triggered by frustration or confusion
- Wandering, as the person aimlessly walks, sometimes trying to “go home” even when already there
- Sundowning—increased confusion and agitation in the late afternoon and evening
- Hallucinations (seeing things that aren’t there) and delusions (false beliefs, such as that someone is stealing from them)
- Sleep disturbances, with daytime napping and nighttime wakefulness
Practical help becomes essential for many daily activities—choosing appropriate clothing, managing bathroom needs, preparing food[62] .
Severe Alzheimer’s Dementia
In the final stage, the brain can no longer sustain basic bodily functions. The person loses the ability to communicate meaningfully, though occasional words or phrases may still emerge. They require full assistance with all activities of daily living—eating, dressing, bathing, toileting .
Physical changes include:
- Loss of mobility—first needing assistance walking, then becoming chair-bound, then bed-bound
- Incontinence of bladder and bowel
- Difficulty swallowing, leading to risk of aspiration pneumonia
- Increased susceptibility to infections, particularly pneumonia and urinary tract infections
Death typically results not from Alzheimer’s itself but from complications like pneumonia, infection, or the cumulative effects of immobility. The disease duration from diagnosis to death averages 4-8 years, though ranges from 3 to 20 years are possible depending on age at onset and other health factors[63] .
Part VII: The Diagnostic Journey
The Clinical Evaluation
Diagnosing Alzheimer’s disease has traditionally been a process of exclusion—ruling out other possible causes of cognitive decline before concluding that Alzheimer’s is the culprit. Today, that is changing, as biological markers allow us to detect the disease itself rather than just its symptoms[64] .
A comprehensive diagnostic evaluation typically includes:
Clinical history—The doctor interviews the patient and, crucially, a family member or close friend who can provide perspective on changes over time. When did symptoms begin? How have they progressed? How do they affect daily function?
Cognitive testing—Brief screening tools like the Mini-Mental State Examination (MMSE) or Montreal Cognitive Assessment (MoCA) provide a snapshot of cognitive function across domains. More comprehensive neuropsychological testing may be used for complex cases or to establish a baseline .
Physical and neurological examination—This assesses general health and looks for signs of other neurological conditions that might explain symptoms.
Brain imaging—Structural MRI can reveal patterns of brain atrophy characteristic of Alzheimer’s, particularly shrinkage in the hippocampus and medial temporal lobe. It also rules out other causes like tumors, strokes, or fluid build[65]up .
The Biological Revolution
The most significant advance in Alzheimer’s diagnosis has been the development of biomarkers—biological measurements that indicate the presence of disease pathology.
Positron emission tomography (PET) scanning can now visualize amyloid and tau directly in the living brain. Amyloid PET tracers bind to beta-amyloid plaques, lighting them up on the scan. Tau PET tracers do the same for neurofibrillary tangles. These scans can detect pathology years before symptoms appear and help distinguish Alzheimer’s from other dementias[66] .
Cerebrospinal fluid (CSF) analysis measures amyloid and tau proteins in the fluid that bathes the brain and spinal cord. In Alzheimer’s disease, amyloid levels in CSF are low (because it’s trapped in plaques in the brain rather than circulating freely), while tau and phosphorylated tau levels are high (reflecting neuronal damage and tangle formation)[67] .
Blood biomarkers are the newest frontier. Highly sensitive assays can now measure specific forms of tau (particularly p-tau217) and ratios of amyloid species in blood samples with remarkable accuracy. A 2025 study showed that combining plasma p-tau217 with brief cognitive tests achieved excellent diagnostic performance, potentially allowing much broader access to biomarker information without requiring PET scans or lumbar punctures[68][69]data-cite-text=”https://www.neurologylive.com/view/biomarker-data-across-studies-support-disease-targeted-effects-valiltramiprosate” [69]class=”js–wpm-format-cite”> [69].
The ATN Framework
Modern Alzheimer’s diagnosis increasingly uses the ATN framework, which categorizes individuals based on three biomarker categories[70] :
A for Amyloid—Is amyloid pathology present? (measured by PET or CSF)
T for Tau—Is tau pathology present? (measured by PET or CSF phosphorylated tau)
N for Neurodegeneration—Is there evidence of neuronal injury? (measured by MRI atrophy, FDG-PET hypometabolism, or CSF total tau)
An individual might be A+T+N+ (all three positive, indicating Alzheimer’s with neurodegeneration), A+T-N- (amyloid positive but no tau or neurodegeneration yet—perhaps preclinical disease), or other combinations that suggest different pathologies or stages.
This framework shifts the definition of Alzheimer’s from a clinical syndrome (dementia with certain features) to a biological construct (presence of specific pathology). It allows diagnosis at earlier stages and enables more precise enrollment in clinical trials targeting specific pathologies[71] .
Part VIII: The Treatment Landscape
Symptomatic Treatments
For decades, the only available treatments for Alzheimer’s addressed symptoms without modifying the underlying disease. These medications remain important tools, though their benefits are modest and temporary[72] .
Cholinesterase inhibitors (donepezil, rivastigmine, galantamine) work by boosting levels of acetylcholine, a neurotransmitter critical for memory and learning that becomes depleted in Alzheimer’s disease. These drugs can temporarily improve symptoms or slow decline in some patients, particularly in mild to moderate stages[73] .
Memantine works differently, regulating glutamate activity to protect neurons from overexcitation. It’s used in moderate to severe Alzheimer’s, often in combination with cholinesterase inhibitors[74] .
Neither class of drugs stops disease progression. They provide symptomatic relief for months to a few years, after which decline resumes its course.
The Anti-Amyloid Revolution
After decades of failed trials, the first disease-modifying therapies for Alzheimer’s have recently reached the market. These are anti-amyloid antibodies—laboratory-made immune proteins designed to bind to beta-amyloid and tag it for clearance by the brain’s immune cells[75] .
Several such antibodies have been tested:
Aducanumab and lecanemab target various forms of amyloid, including plaques and soluble oligomers. Clinical trials have shown they can significantly reduce amyloid burden in the brain and slow cognitive decline—by about 25-35% over 18 months in the case of lecanemab. The effect is modest but meaningful: more time in milder stages, delayed progression to more severe impairment .
Donanemab has shown similar benefits, with the greatest effects in people with early disease and low to intermediate tau levels—supporting the idea that intervening early, before tau spreads widely, is critical[76] .
Valiltramiprosate represents a different approach—an oral drug that inhibits amyloid oligomer formation. Recent biomarker data shows it reduces p-tau217 levels (a marker of disease activity) and correlates with cognitive benefits and protection against brain atrophy, particularly in APOE4 carriers with mild cognitive impairment[77] .
These treatments come with significant challenges. They require regular intravenous infusions. They carry risks of amyloid-related imaging abnormalities (ARIA) —brain swelling or microhemorrhages that must be monitored with MRI. And they are not cures; they slow progression but do not stop it. Yet they represent a historic breakthrough: proof that modifying the underlying disease process is possible[78] .
Beyond Amyloid
While anti-amyloid therapies dominate current headlines, other approaches are in development:
Anti-tau therapies aim to clear tau aggregates or prevent their spread between neurons. These are in earlier stages of testing but may complement anti-amyloid treatments.
Anti-inflammatory drugs target the neuroinflammation that contributes to neurodegeneration. Some repurposed drugs with anti-inflammatory properties are being tested.
Metabolic approaches address the energy failure in Alzheimer’s brains. These include ketogenic interventions, insulin sensitizers, and treatments targeting mitochondrial function[79] .
Combination therapies will likely be needed, analogous to cancer treatment—attacking the disease through multiple mechanisms simultaneously.
Part IX: Prevention—The Power of Lifestyle
The Modifiable Risk Factors
If Alzheimer’s begins decades before symptoms appear, then the decades before symptoms offer an opportunity for prevention. Epidemiologic research has identified numerous modifiable risk factors that influence Alzheimer’s risk[80][81]data-cite-text=”https://neurologytoday.aan.com/doi/full/10.1097/01.NT.0000604232.10286.3d?ContribAuthorRaw=Collins%2C+Thomas+R&af=R&sortBy=Earliest&mi=4ugont&content=netod&ConceptID=502206&target=netod” [81]class=”js–wpm-format-cite”> [81].
The Lancet Commission on Dementia Prevention has estimated that up to 40% of dementia cases worldwide might be prevented or delayed by addressing 12 modifiable risk factors across the lifespan:
Early life (≤ age 45):
- Less education—reduces cognitive reserve
Midlife (age 45-65):
- Hypertension—damages cerebral blood vessels
- Obesity—promotes inflammation and metabolic dysfunction
- Hearing loss—increases cognitive load and social isolation
- Traumatic brain injury—direct neuronal damage
- Excessive alcohol consumption—neurotoxic effects
Later life (age 65+):
- Smoking—vascular damage and oxidative stress
- Depression—chronic stress and inflammation
- Social isolation—reduces cognitive stimulation
- Physical inactivity—reduces blood flow and neurotrophins
- Air pollution—neuroinflammatory effects
- Diabetes—vascular damage and metabolic stress
Addressing these factors doesn’t guarantee prevention, but it shifts the risk curve favorably.
The Mediterranean Advantage
Among dietary patterns, the Mediterranean diet has accumulated the strongest evidence for brain protection. Characterized by high intake of vegetables, fruits, legumes, whole grains, fish, and olive oil; moderate wine consumption; and low intake of red meat and processed foods, this pattern seems to benefit the brain through multiple mechanisms[82] .
A 2025 study examining the interaction between diet and genetics found that adherence to a Mediterranean-style diet was associated with lower dementia risk and slower cognitive decline. Notably, the protective effect was strongest in people with the highest genetic risk—those carrying two copies of the APOE4 allele. For this group, following the Mediterranean diet made a particularly large difference[83] .
How does diet help? Potential mechanisms include:
- Reducing inflammation throughout the body and brain
- Providing antioxidants that combat oxidative stress
- Improving vascular health, maintaining cerebral blood flow
- Supporting healthy metabolism and insulin sensitivity
- Providing specific nutrients (omega-3 fatty acids, polyphenols) that support neuronal function
The message is empowering:even for those with the strongest genetic risk, lifestyle choices matter. Genes are not destiny.
The Limits of Lifestyle
The interaction between genetics and lifestyle is complex. A 2019 study using data from the Rotterdam Study found that while healthy lifestyle habits could substantially reduce dementia risk for people with low or intermediate genetic risk, the benefits were less clear for those at highest genetic risk (APOE4/4 homozygotes). For this group, the 15-year risk of dementia was similar regardless of lifestyle profile[85] .
This doesn’t mean lifestyle doesn’t matter for high-risk individuals. Other studies have found benefits even for APOE4 carriers[86] . And the Rotterdam Study authors noted that intervening earlier—in midlife rather than later—might be necessary for those with the highest genetic risk. The message is not hopelessness but timing: if you carry high-risk genes, you may need to start prevention efforts earlier and pursue them more diligently[87] .
Part X: The Future Frontier
The Promise of Earlier Intervention
The long preclinical phase of Alzheimer’s disease—the 15-20 years during which pathology accumulates silently—offers an unprecedented opportunity. If we can identify who is on the path to Alzheimer’s decades before symptoms appear, we might intervene to delay or even prevent symptom onset entirely[88] [89].
This is the logic behind secondary prevention trials, which enroll cognitively normal individuals who are biomarker-positive (amyloid-positive but asymptomatic) and test whether anti-amyloid treatments can prevent cognitive decline. The success of these trials would transform Alzheimer’s from a disease we treat after symptoms appear to one we prevent before they ever emerge.
Blood biomarkers are key to this vision. If a simple blood test can identify who needs further evaluation and possible treatment, screening at scale becomes feasible. A 2025 study demonstrated that combining plasma p-tau217 with brief cognitive tests in primary care settings could identify individuals needing specialist referral with high accuracy—a model for population-level screening[90].
The Combination Therapy Era
Just as cancer treatment has moved from single agents to combination regimens targeting multiple pathways, Alzheimer’s treatment will likely evolve toward combination therapy[91] .
A future treatment regimen might include:
- An anti-amyloid antibody to clear plaques
- An anti-tau agent to prevent tangle spread
- An anti-inflammatory drug to calm microglial activation
- A metabolic enhancer to support neuronal energy production
- Lifestyle interventions to address vascular and other risk factors
Finding the right combinations, sequences, and timing for different patient subgroups will require extensive research. But the goal is clear: to attack the disease from multiple angles simultaneously.
Beyond Proteins
While amyloid and tau dominate current research, other frontiers are opening:
The gut-brain axis—Emerging evidence suggests that gut microbiota composition influences brain health through immune, metabolic, and neural pathways. Manipulating the gut microbiome might offer novel preventive or therapeutic approaches[92] .
The viral hypothesis—Some research suggests that certain viruses (herpes simplex virus type 1, among others) might trigger or accelerate Alzheimer’s pathology in genetically susceptible individuals. If confirmed, this could open avenues for antiviral prevention .
Personalized medicine—Genetic profiling, biomarker analysis, and risk factor assessment might eventually allow truly personalized approaches: knowing that a particular individual’s Alzheimer’s risk is driven primarily by inflammation suggests anti-inflammatory strategies; metabolic drivers suggest metabolic interventions; and so on[93] [94] .
The Ethical Dimensions
As we move toward earlier diagnosis and potential presymptomatic intervention, ethical questions multiply:
Who should be tested, and when? Should asymptomatic individuals undergo biomarker screening? What are the psychological consequences of knowing you have Alzheimer’s pathology decades before symptoms might appear?
How do we ensure equitable access? If expensive new treatments become available, will they be accessible only to the wealthy? How do we address disparities in risk and care?
What does it mean to “prevent” a disease when the prevention itself carries risks? The anti-amyloid antibodies can cause brain swelling and bleeding. At what point do the benefits outweigh the risks for asymptomatic individuals?
These questions have no easy answers. They will require ongoing dialogue among researchers, clinicians, patients, families, and society at large.
Epilogue: The Stories Within the Science
Auguste Deter died in 1906, never knowing that her suffering would launch a century of scientific inquiry. Her brain, preserved on slides in Munich, still holds the plaques and tangles that Alois Alzheimer first described—physical evidence of the disease that now bears his name.
In the years since, we have learned an enormous amount. We know the proteins involved, the genes that influence risk, the stages of pathology and symptom progression. We have developed biomarkers that can detect the disease in living people, and treatments that can slow its course. We stand at the threshold of an era where prevention may become possible.
But for all our scientific progress, Auguste’s words still resonate: “I have lost myself.”
Alzheimer’s disease is not just about proteins and plaques, genes and biomarkers. It is about the gradual dissolution of a self—the slow erasure of memories, relationships, skills, and stories that together constitute a human life. It is about the spouse who becomes a stranger, the parent who cannot recognize their child, the brilliant mind that slowly dims.
And it is also about the caregivers who watch this process unfold, day after day, year after year. The daughter who patiently answers the same question for the hundredth time. The husband who learns to interpret his wife’s nonverbal cues when words fail. The family that finds new ways to connect and love even as the disease progresses.
The science matters because it offers hope—hope for better treatments, for prevention, for eventual cure. But the stories matter too. They remind us why this work is important. They keep us focused on the ultimate goal: preserving not just brains, but lives; not just cognitive function, but personhood.
Auguste Deter lost herself to a disease that, in 1901, had no name. Today, we know her enemy. And we are learning, slowly but surely, how to fight back.
Bibiliography
The following links correspond to the primary research articles and academic sources cited throughout this entry.
- [1] https://pmc.ncbi.nlm.nih.gov/articles/PMC11568893/
- [2] https://www.alz.org/alzheimers-dementia/research_progress/milestones?form=FUNJQDBBMMH
- [3] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [4] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [5] https://pubmed.ncbi.nlm.nih.gov/41513640/
- [6] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [7]
- [8] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [9]
- [10] https://pmc.ncbi.nlm.nih.gov/articles/PMC11568893/
- [11] https://pmc.ncbi.nlm.nih.gov/articles/PMC11568893/
- [12] https://pmc.ncbi.nlm.nih.gov/articles/PMC11568893/
- [13] https://www.alz.org/alzheimers-dementia/research_progress/milestones?form=FUNJQDBBMMH
- [14] https://pmc.ncbi.nlm.nih.gov/articles/PMC11568893/
- [15] https://www.alz.org/alzheimers-dementia/research_progress/milestones?form=FUNJQDBBMMH
- [16] https://www.alz.org/alzheimers-dementia/research_progress/milestones?form=FUNJQDBBMMH
- [17] https://pmc.ncbi.nlm.nih.gov/articles/PMC11568893/
- [18] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [19] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [20] https://pubmed.ncbi.nlm.nih.gov/41513640/
- [21]
- [22] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [23]
- [24] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [25] https://pubmed.ncbi.nlm.nih.gov/41513640/
- [26] https://pubmed.ncbi.nlm.nih.gov/41513640/
- [27] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [28] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [29] https://www.ukdri.ac.uk/news-and-events/vulnerable-neuronal-subsets-identified-early-alzheimers
- [30] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [31] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [32] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [33]
- [34] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [35] https://pubmed.ncbi.nlm.nih.gov/41513640/
- [36] https://www.ukdri.ac.uk/news-and-events/vulnerable-neuronal-subsets-identified-early-alzheimers
- [37] https://www.ukdri.ac.uk/news-and-events/vulnerable-neuronal-subsets-identified-early-alzheimers
- [38] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [39] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [40] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [41] https://www.alz.org/alzheimers-dementia/research_progress/milestones?form=FUNJQDBBMMH
- [42] https://www.alz.org/alzheimers-dementia/research_progress/milestones?form=FUNJQDBBMMH
- [43] https://www.alz.org/alzheimers-dementia/research_progress/milestones?form=FUNJQDBBMMH
- [44] https://www.alz.org/alzheimers-dementia/research_progress/milestones?form=FUNJQDBBMMH
- [45] https://neurologytoday.aan.com/doi/full/10.1097/01.NT.0000604232.10286.3d?ContribAuthorRaw=Collins%2C+Thomas+R&af=R&sortBy=Earliest&mi=4ugont&content=netod&ConceptID=502206&target=netod
- [46] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [47] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [48] https://neurologytoday.aan.com/doi/full/10.1097/01.NT.0000604232.10286.3d?ContribAuthorRaw=Collins%2C+Thomas+R&af=R&sortBy=Earliest&mi=4ugont&content=netod&ConceptID=502206&target=netod
- [49] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [50] https://neurologytoday.aan.com/doi/full/10.1097/01.NT.0000604232.10286.3d?ContribAuthorRaw=Collins%2C+Thomas+R&af=R&sortBy=Earliest&mi=4ugont&content=netod&ConceptID=502206&target=netod
- [51] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [52] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [53]
- [54] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
- [55] https://pubmed.ncbi.nlm.nih.gov/40866545/
- [56] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [57] https://pubmed.ncbi.nlm.nih.gov/40866545/
- [58] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [59] https://pubmed.ncbi.nlm.nih.gov/40866545/
- [60] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [61] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [62] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [63] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [64] https://pubmed.ncbi.nlm.nih.gov/40866545/
- [65] https://pubmed.ncbi.nlm.nih.gov/40866545/
- [66] https://pubmed.ncbi.nlm.nih.gov/40866545/
- [67] https://pubmed.ncbi.nlm.nih.gov/40866545/
- [68] https://pubmed.ncbi.nlm.nih.gov/40866545/
- [69] https://www.neurologylive.com/view/biomarker-data-across-studies-support-disease-targeted-effects-valiltramiprosate
- [70] https://pubmed.ncbi.nlm.nih.gov/40866545/
- [71] https://pubmed.ncbi.nlm.nih.gov/40866545/
- [72] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [73] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [74] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [75] https://www.neurologylive.com/view/biomarker-data-across-studies-support-disease-targeted-effects-valiltramiprosate
- [76] https://www.neurologylive.com/view/biomarker-data-across-studies-support-disease-targeted-effects-valiltramiprosate
- [77] https://www.neurologylive.com/view/biomarker-data-across-studies-support-disease-targeted-effects-valiltramiprosate
- [78] https://www.neurologylive.com/view/biomarker-data-across-studies-support-disease-targeted-effects-valiltramiprosate
- [79] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [80] https://fe.prod.content.healthgrades.com/pro/mediterranean-diet-may-help-slow-cognitive-decline-in-those-at-high-genetic-risk-alzheimers?tpc=treating-autoimmune-arthritis
- [81] https://neurologytoday.aan.com/doi/full/10.1097/01.NT.0000604232.10286.3d?ContribAuthorRaw=Collins%2C+Thomas+R&af=R&sortBy=Earliest&mi=4ugont&content=netod&ConceptID=502206&target=netod
- [82] https://fe.prod.content.healthgrades.com/pro/mediterranean-diet-may-help-slow-cognitive-decline-in-those-at-high-genetic-risk-alzheimers?tpc=treating-autoimmune-arthritis
- [83] https://fe.prod.content.healthgrades.com/pro/mediterranean-diet-may-help-slow-cognitive-decline-in-those-at-high-genetic-risk-alzheimers?tpc=treating-autoimmune-arthritis
- [84] https://fe.prod.content.healthgrades.com/pro/mediterranean-diet-may-help-slow-cognitive-decline-in-those-at-high-genetic-risk-alzheimers?tpc=treating-autoimmune-arthritis
- [85] https://neurologytoday.aan.com/doi/full/10.1097/01.NT.0000604232.10286.3d?ContribAuthorRaw=Collins%2C+Thomas+R&af=R&sortBy=Earliest&mi=4ugont&content=netod&ConceptID=502206&target=netod
- [86] https://fe.prod.content.healthgrades.com/pro/mediterranean-diet-may-help-slow-cognitive-decline-in-those-at-high-genetic-risk-alzheimers?tpc=treating-autoimmune-arthritis
- [87] https://neurologytoday.aan.com/doi/full/10.1097/01.NT.0000604232.10286.3d?ContribAuthorRaw=Collins%2C+Thomas+R&af=R&sortBy=Earliest&mi=4ugont&content=netod&ConceptID=502206&target=netod
- [88] https://pubmed.ncbi.nlm.nih.gov/40866545/
- [89]
- [90] https://pubmed.ncbi.nlm.nih.gov/40866545/
- [91] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [92] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [93] https://www.sciencedirect.com/science/article/abs/pii/S0344033825003024
- [94] https://www.sciencedirect.com/science/article/abs/pii/S0306452225010486
External Links
• National Institute on Aging — Alzheimer’s Disease Information
https://www.nia.nih.gov/health/alzheimers
• Alzheimer’s Association — Alzheimer’s & Dementia Resource Center
https://www.alz.org
• World Health Organization — Dementia Fact Sheet
https://www.who.int/news-room/fact-sheets/detail/dementia
• PubMed — Alzheimer’s Disease Research Database
https://pubmed.ncbi.nlm.nih.gov/?term=alzheimers+disease
• National Institute of Neurological Disorders and Stroke — Alzheimer’s Disease Information
https://www.ninds.nih.gov/health-information/disorders/alzheimers-disease
• Alzheimer’s Disease International
https://www.alzint.org
• ClinicalTrials.gov — Alzheimer’s Disease Clinical Studies
https://clinicaltrials.gov/search?cond=Alzheimer%20Disease
Utopedia entry last updated: March 2026
This article is intended for informational purposes and reflects the scientific understanding at the time of publication. Medical knowledge evolves rapidly; readers with specific concerns about Alzheimer’s disease should consult healthcare professionals for personalized guidance.